Hello again, Ramin Rak here, welcoming you back to my blog.
As a spine and brain specialist, I deal with an increasingly large number of patients who suffer from traumatic brain injury, or TBI.

Ramin Rak recommends seeking medical help if you experience any of these symptoms taking a blow to the head.
According to the CDC, TBI contributes to a substantial number of deaths or permanent disability annually.
A TBI occurs when an individual experiences trauma to the head that disrupts the brain’s normal function. The severity of a TBI can vary from mild to severe, but experts like myself encourage patients to treat all forms of TBI very seriously.
Perhaps the most common type of TBI is a concussion. While they are not typically life threatening, their effects can be serious. The CDC recommends contacting a health care professional if you begin to experience any of the following after a blow to the head:
- Headache that won’t go away
- Decreased coordination
- Vomiting
- Slurred speech
- Drowsiness
- Lose consciousness
- Unusual behavior
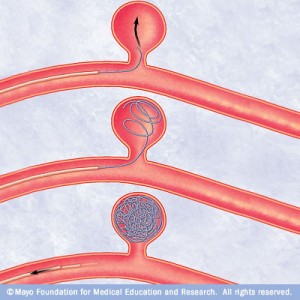
With proper treatment, it is unlikely a concussion will have a lasting effect. Contrary, there are two types of TBI that have the potential to cause long terms effects and even death. Closed head injuries, often due to falls or vehicle crashes, occur when the brain moves within the skill. Penetrating injuries occur when an object enters the skull, such as firearm injuries. Statistics show that after a severe TBI, 43% of patients hospitalized suffer from short or long term issues a year later. These can include:
- Loss of cognitive function, such as memory and attention.
- Loss of motor function, including weakness and poor coordination.
- Sensation; for example impaired perception, hearing, or vision.
- Emotional changes, including depression, aggression, and lack of impulse control.
The consequences of a severe TBI can affect an individual’s life, but there are steps that can be taken to limit the injuries impact. The CDC recommends primary intervention, early management, and treatment of severe TBI for best results.
Learn more about me, Ramin Rak, and my unique skill sets here: http://www.linkedin.com/in/raminrak, and here http://raminrak.com/ramin-rak-traumatic-brain-injury-treatments/.